Key takeaways
By 2045, the transformation of the Swiss hospital landscape is no longer a hypothesis but a structural necessity. Studies converge on the same point: without reorganising care networks, optimising resources and modernising care models, the quality, accessibility and financial sustainability of the system will be durably weakened. Digital is not a miracle solution, but an essential condition for steering this transformation in a coherent and measurable way. Institutions that invest in digital tools genuinely aligned with their core activities will gain a decisive advantage in adapting to the changes ahead. Conversely, the accumulation of non-integrated solutions risks increasing complexity rather than reducing it.
2026: from observation to transformation of the Swiss hospital system

The beginning of 2026 marks a pivotal moment. The Swiss hospital system has entered a phase of sustained pressure that goes far beyond the cyclical effects observed in recent years. The continuous rise in costs, the chronic shortage of qualified staff, the ageing of the population and the growing demands regarding quality, safety and accessibility of care are placing simultaneous pressure on the entire system. In this context, the question is no longer whether the Swiss hospital landscape must transform, but how to do so in a realistic, sustainable and coordinated way.
This is precisely what the forward-looking study by PwC on the evolution of the Swiss hospital landscape by 2045 highlights. At the same time, recent analyses on the digital transformation of healthcare in Switzerland — whether from the Confederation (the DigiSanté programme), strategic consulting firms such as Boston Consulting Group, or national ecosystems like digitalswitzerland — converge on a complementary conclusion: without a robust, interoperable digital foundation aligned with professional practices, no structural transformation can truly succeed.
This article proposes a cross-analysis of these reference works. It shows how the strategic directions identified for the 2045 horizon are already translating today into operational digital initiatives and into the development of custom business software adapted to the realities of Swiss hospitals.
A widely shared assessment of the limitations of the current model
The PwC study on the Swiss hospital landscape looking ahead to 2045 is part of a forward-looking modelling approach. It analyses different evolution scenarios and assesses their effects across three key dimensions: the quality and safety of care, the financial sustainability of the system, and accessibility for the population. One of the study’s central findings is the identification of persistent structural imbalances.
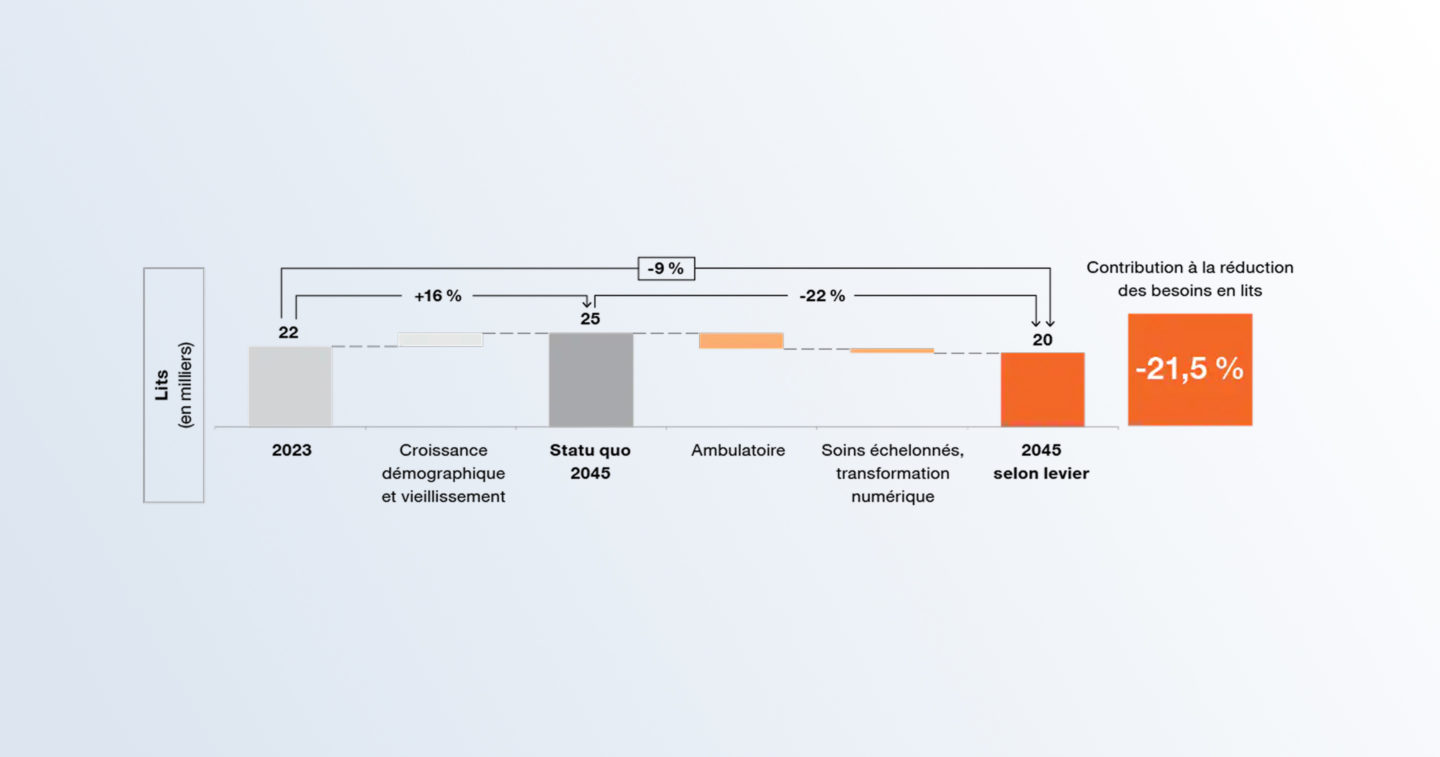
Switzerland faces an uneven distribution of hospital capacity: some regions experience overcapacity, while others struggle to maintain an adequate level of services. Furthermore, a small number of hospitals are becoming increasingly systemically important, both in terms of patient volumes and specialisation. This trend raises questions about the overall resilience of the system and its ability to absorb future shocks.
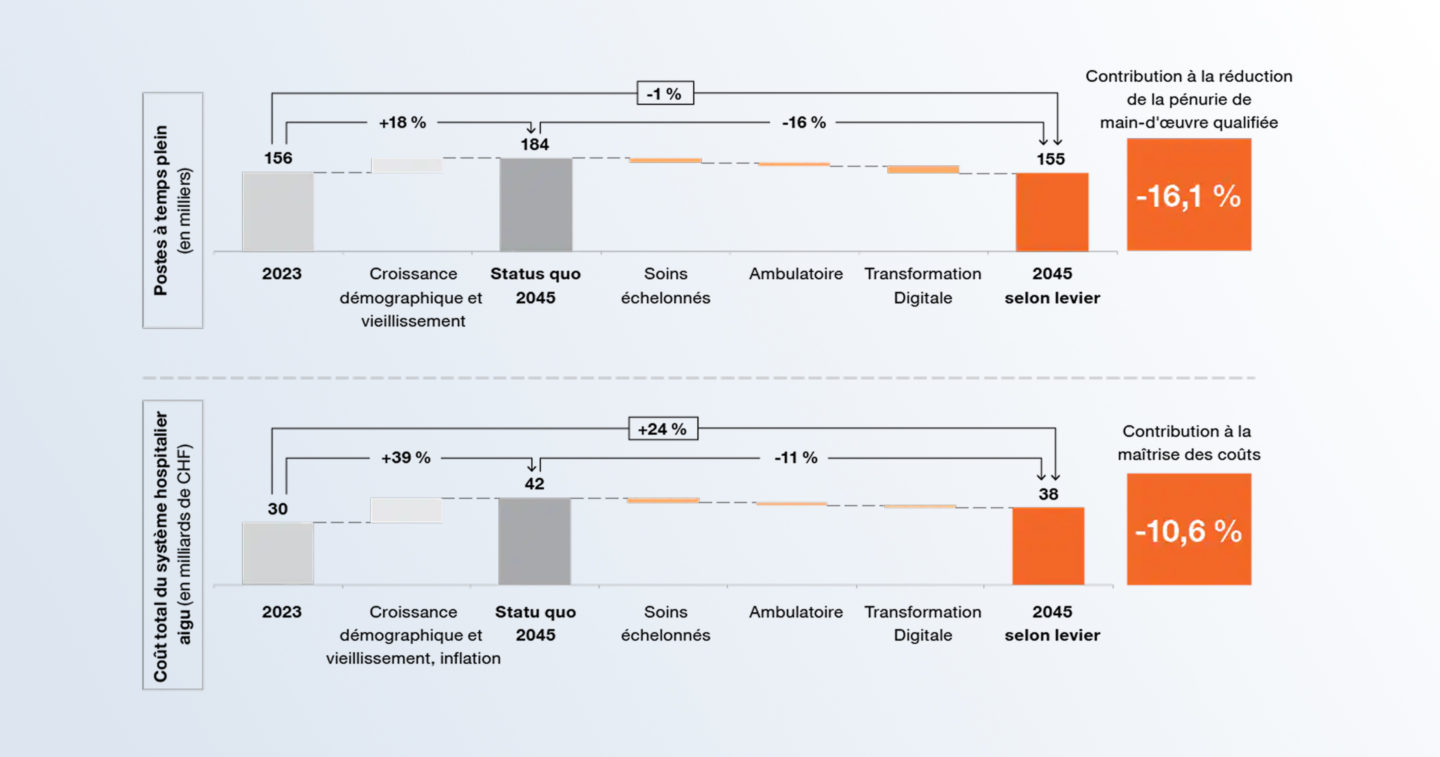
The study also highlights the limitations of a model still largely based on hospitals operating as autonomous entities. PwC explicitly advocates for a transition towards integrated care networks, capable of coordinating services, pooling certain functions, and guiding patients more efficiently within the system.
Three levers for transformation by 2045

The scenarios studied are based on three major, closely interdependent levers for transformation.
The first concerns the reorganisation of the hospital network and care provision. This involves better distribution of capacities, strengthening the specialisation of certain sites, and developing sustainable collaborations between institutions. PwC considers that such a reorganisation could generate significant gains in care quality while reducing costly redundancies.
The second lever focuses on optimising processes and resource utilisation. Faced with a persistent staff shortage, the challenge is no longer solely financial. It involves reducing administrative burden, streamlining internal workflows, and improving working conditions for healthcare professionals to maintain the attractiveness of hospital professions.
The third lever relates to the modernisation of care models. The shift towards outpatient care, the development of integrated services, and the expansion of telemedicine are identified as key axes to meet future population needs while controlling costs. The study emphasises that these changes are inseparable from improved coordination among hospital, outpatient, and community actors.
These three levers share a common prerequisite: precise management driven by data, made possible through reliable digital processes and enhanced interoperability between systems.
The digital transformation of healthcare in Switzerland: a committed but fragmented movement
Work on digital healthcare in Switzerland presents a mixed picture. On one hand, Switzerland has strong innovation potential and has seen numerous initiatives emerge since the Covid‑19 pandemic. Telemedicine, remote monitoring solutions, and appointment booking platforms have developed significantly, driven by cost constraints, staff shortages, and generally positive user feedback.
On the other hand, several benchmark studies highlight a persistent lag compared with countries such as Denmark or Estonia. The Boston Consulting Group report, Advancing the Swiss Healthcare System, points out limitations linked to fragmented systems, insufficient interoperability, and the still limited use of health data in organisational management.
Digitalswitzerland barometers confirm this assessment. They show that healthcare professionals are generally supportive of digitisation but criticise the proliferation of non-integrated solutions, which generate additional administrative workload (https://digitalswitzerland.com/fr/un-systeme-de-sante-numerique-suisse-ce-quen-pense-la-population/).
DigiSanté and the Swiss Health Data Space: a structuring framework at the national level
The federal DigiSanté programme is currently the most structuring initiative for healthcare digitalisation in Switzerland. Backed by funding of around 392 million francs for the 2025–2034 period, it aims to catch up with the digital lag in the Swiss healthcare system through a three-phase roadmap: establishment of standards and infrastructures (2025–2027), deployment of services and interfaces (2028–2030), and finally optimisation and consolidation (2031–2034).
Within this framework, DigiSanté is structured around four complementary strategic objectives: digitise, orchestrate, standardise, and embed. They take into account the specificities of the Swiss healthcare system, build on existing initiatives such as the DEP, and integrate, where relevant, international developments.
Digitise aims to lay the foundations for digital transformation and support concrete projects that add value to care. Orchestrate focuses on coordinating stakeholders and initiatives to strengthen collective efficiency. Standardise enables secure and interoperable data exchange, notably through recognised standards such as SNOMED CT, HL7 FHIR, IHE, DICOM, or openEHR. Finally, embed seeks to evolve the necessary legal frameworks to ensure this transformation is sustainably implemented at cantonal and federal levels.
A central pillar of this strategy is the creation of the Swiss Health Data Space, designed as a decentralised yet interoperable environment for secure health data exchange. Its objectives are multiple: reducing administrative burden, improving quality of care, enhancing transparency, and facilitating research, all while meeting the high standards of data protection.
https://www.digisante.admin.ch/dam/fr/sd-web/MRFsoZIQ2HCP/Rapport%20DigiSant%C3%A9%202025.pdf
Focus on romandy: specific challenges and levers for action
 Opinion surveys conducted by digitalswitzerland show that romandy exhibits a perceived digital maturity slightly lower than that observed in german-speaking switzerland. Concerns regarding data protection and accessibility of digital services are also more pronounced. This observation, however, should be put into perspective.
Opinion surveys conducted by digitalswitzerland show that romandy exhibits a perceived digital maturity slightly lower than that observed in german-speaking switzerland. Concerns regarding data protection and accessibility of digital services are also more pronounced. This observation, however, should be put into perspective.
Romandy hosts several major players in digital health, notably the university hospitals of geneva and vaud, as well as academic hubs and specialised continuing education programmes. The programmes offered by unisanté in lausanne, for example, explicitly aim to address the digital skills gap among healthcare professionals and support the implementation of regional transformation projects (https://www.unisante.ch/fr/formation-recherche/formation/formation-continue/catalogue-formations-continues/sante-digitale).
In this context, the creation of the romandy digital health interest group seeks to provide a shared regional space dedicated to digital health. Its ambition is to give a collective voice to field actors and strengthen their ability to position themselves on cantonal and federal strategic issues.
The group aims to enhance cooperation in romandy by facilitating peer exchanges, supporting the emergence of cross-cutting projects, and promoting a common approach to the digital challenges facing the healthcare system. It operates in a collaborative logic, connected to existing initiatives, and oriented towards sharing experiences, practices, and digital priorities.
Its functioning is intentionally light and pragmatic, with no leadership role, no operational mandate, and no decision-making power. The group’s mission is primarily to showcase romandy expertise, strengthen collaborations, and provide a shared romandy contribution to digital health.
From strategic framework to concrete tools
One of the cross-cutting lessons from all these studies is that transformation cannot succeed without an operational translation closely aligned with real-world workflows. Friction points are now well identified: inter‑facility coordination, capacity planning, patient pathway management, clinical and administrative documentation, and regulatory reporting.
In this context, generic digital solutions quickly reach their limits. The healthcare system requires solutions that can evolve with funding models, regulatory requirements, and the specific structures of each care network. This entails bespoke business software, integrated with existing systems and aligned with the actual workflows of clinical, logistical, financial, and HR teams.
Apptitude’s positioning
Apptitude SA supports organisations facing complex and highly regulated environments, where technology choices have long-term strategic implications. In the hospital sector, our approach relies on the levers identified by reference studies (reorganisation of care provision, optimisation of resources, modernisation of care models) to co-design, with management and operational teams, software solutions truly adapted to the realities on the ground.
This approach prioritises integration with existing systems, data security, user ergonomics, and solution scalability, aiming to support the transformation of the Swiss healthcare system over the long term, up to 2045.
In this context, Apptitude SA also works on projects subject to medical device regulations (MDS), particularly with regard to the IEC 62304 standard, which governs the lifecycle of medical device software. This standard requires software categorisation according to different safety classes (A, B, C) and rigorous risk management, translated into a set of requirements covering the entire software development lifecycle: planning, requirements analysis, architectural and detailed design, implementation, unit testing, integration and testing, system software validation, up to software release. These activities are orchestrated according to a “V-model” verification and validation approach, ensuring long-term control of quality, safety, and compliance, notably through maintenance, configuration, and bug resolution plans, as well as full traceability of activities and deliverables within a quality management system (QMS).
Apptitude’s expertise can be mobilised at different stages of this process, and the deliverables produced are designed to be directly usable in the preparation of regulatory documentation. Since IEC 62304 does not fully cover all regulatory requirements applicable to medical devices, Apptitude also integrates relevant complementary standards, such as IEC 62366 for usability engineering and human factors, ISO 13485 for regulatory quality management systems, ISO 14971 for risk management, and IEC 62443 (notably series 4-2) for cybersecurity concerns in software and industrial systems.
Conclusion
Prospective analyses of digital health converge towards an unambiguous conclusion: the transformation of the Swiss hospital system is inevitable. Digital technology is neither the cause nor the ultimate goal, but a structural condition for success when designed as a tool serving professional practices and strategy.
For healthcare decision-makers, the challenge in the coming years will be to translate these strategic frameworks into concrete operational capabilities without adding unnecessary complexity. It is in this space, at the interface of vision, organisation, and technology, that Apptitude SA positions itself as a long-term partner.
Main sources
PwC – Étude prospective sur le paysage hospitalier suisse à l’horizon 2045
Boston Consulting Group – Transformation numérique du système de santé suisse
Programme fédéral DigiSanté – Rapport 2025
Digital Health Report 2025/2026 – Poste suisse
digitalswitzerland – Baromètres sur la santé numérique
FMCH – Étude sur la numérisation du système de santé suisse
Unisanté – Formations continues en santé digitale